Introduction to Vitrectomy Surgery
What Is Vitrectomy?
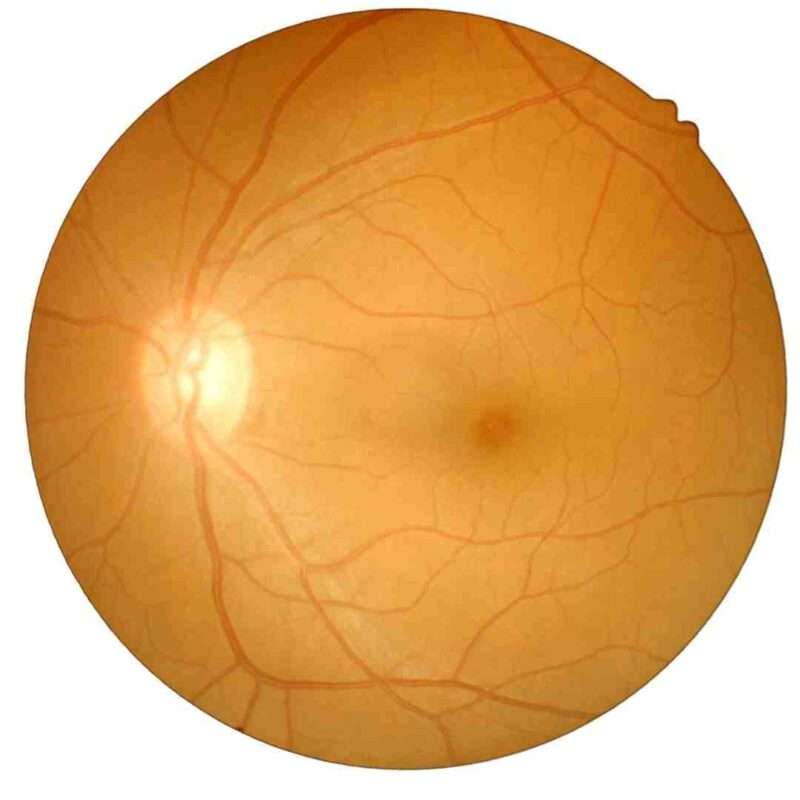
Surgeons perform vitrectomy as a highly specialized procedure to treat disorders affecting the retina and vitreous of the eye. If you imagine the eye as a small globe filled with a clear, gel-like substance, you are picturing the vitreous humor. Over time, disease, injury, or aging can cause this gel to cloud, bleed, or pull on the retina. When that happens, vision becomes distorted, blurry, or even completely lost. A vitrectomy operation involves removing this vitreous gel to allow the surgeon direct access to the retina for repair.
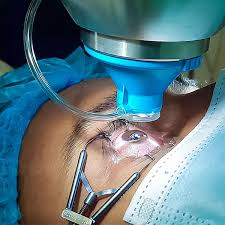
This isn’t a cosmetic procedure. It’s a sight-saving surgery performed by a retinal specialist—an ophthalmologist trained in delicate microsurgical techniques. The surgery is typically done using high-powered microscopes and ultra-fine instruments that enter the eye through tiny incisions. Modern advancements have made vitrectomy far safer and more precise than it was decades ago.
You might wonder why removing something inside the eye doesn’t cause harm.
Once the surgeon removes the vitreous gel, they replace it with a saline solution, gas bubble, or silicone oil to maintain the eye’s shape. Over time, the eye naturally produces fluid and gradually fills the space that the surgeon cleared. Think of it as renovating the inside of a house without damaging its structure—careful, precise, and purposeful.
Vitrectomy has revolutionized the management of complex retinal diseases. Today, it stands as one of the most important procedures in modern ophthalmology, restoring vision and preventing blindness in thousands of patients each year.
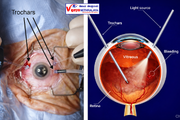
Why This Procedure Is Performed
Doctors do not perform vitrectomy surgery without reason. They typically recommend it when serious eye conditions threaten vision and do not respond to medications or less invasive treatments. The primary goal is to restore clarity, relieve traction on the retina, or remove obstructive material that interferes with sight.
For example, in diabetic retinopathy, fragile blood vessels can leak into the vitreous cavity, causing bleeding known as vitreous hemorrhage. When blood fills the eye, light cannot pass through properly, leading to significant vision loss. In such cases, vitrectomy clears the blood and allows the surgeon to treat the underlying retinal damage.
Another common reason for vitrectomy is retinal detachment. This is a medical emergency where the retina pulls away from the back of the eye. If left untreated, permanent blindness can occur. During vitrectomy, the surgeon repositions the retina and seals it in place using laser or cryotherapy.
Macular holes and epiretinal membranes (macular puckers) are also treated through this procedure. These conditions distort central vision, making reading or recognizing faces difficult. By removing the vitreous and relieving traction, the surgeon can improve visual clarity significantly.
Eye trauma, infections inside the eye (endophthalmitis), and complications from previous surgeries may also require vitrectomy. In short, whenever the vitreous gel becomes part of the problem rather than part of the solution, surgical removal becomes necessary.
Vitrectomy is not about comfort—it’s about preserving one of your most valuable senses. And when vision is at stake, precision matters.
Anatomy of the Eye and the Role of the Vitreous
Structure of the Vitreous Humor
To understand vitrectomy, you need to understand the vitreous humor. Picture a clear, jelly-like substance filling about two-thirds of your eye. That’s the vitreous. It sits between the lens at the front and the retina at the back, acting as a transparent cushion.
The vitreous is composed mainly of water—about 99%—with small amounts of collagen fibers and hyaluronic acid that give it structure. In youth, it has a firm gel consistency. As we age, it gradually liquefies and may shrink. This natural process is known as vitreous degeneration and often leads to floaters.
Despite being clear, the vitreous plays an essential role in maintaining the eye’s shape. It helps keep the retina pressed gently against the back wall of the eye. It also allows light to pass through unobstructed to reach the retina, where visual signals are generated.
However, the vitreous is not firmly attached everywhere. It has strong attachment points around the optic nerve and macula. When it shrinks or pulls away abnormally, it can create traction on the retina. In severe cases, this traction can cause retinal tears or detachment.
Interestingly, the vitreous has no blood supply. That means once it becomes clouded with blood or debris, the body struggles to clear it quickly. This is one reason vitrectomy becomes necessary in cases of persistent hemorrhage.
Understanding the vitreous helps clarify why its removal can solve so many retinal problems. It’s not about removing something vital—it’s about removing a problematic structure that is interfering with vision.
How the Vitreous Affects Vision
Vision depends on clarity. Light must travel smoothly through the cornea, lens, vitreous, and finally reach the retina. If any part of this pathway becomes obstructed, vision suffers.
When the vitreous is clear, it functions almost invisibly. But when it fills with blood, inflammatory cells, scar tissue, or debris, it becomes a barrier. Imagine trying to look through a fogged window—that’s what patients often describe.
Additionally, when the vitreous pulls on the retina, it distorts the retinal surface. This can lead to wavy or blurred central vision. In macular holes, the pulling creates a small defect in the central retina, severely affecting sharp vision.
Floaters are another common vitreous-related issue. While usually harmless, severe floaters can interfere with daily activities. In select cases, vitrectomy may be performed to remove persistent, visually disabling floaters.
In short, while the vitreous plays a structural role, it is not essential for long-term visual function. Once removed and replaced, most patients adapt well without noticing any difference in daily life—except improved clarity.
Common Conditions Treated with Vitrectomy
Retinal Detachment
Retinal detachment is one of the most urgent reasons for vitrectomy surgery. The retina acts like the film in a camera—it captures light and sends signals to the brain. When it detaches, that signal pathway is interrupted.
Symptoms often include flashes of light, sudden floaters, or a curtain-like shadow over vision. Without prompt treatment, permanent vision loss can occur. During vitrectomy, the surgeon removes the vitreous gel that is pulling on the retina, repositions the retina, and seals tears using laser therapy. A gas bubble or silicone oil may then be inserted to hold the retina in place during healing.
This procedure has a high success rate when performed early. The key is immediate medical attention.
Diabetic Retinopathy
Diabetic retinopathy is one of the leading causes of vision loss worldwide, and vitrectomy plays a crucial role in managing its advanced stages. When blood sugar levels remain uncontrolled over time, the tiny blood vessels in the retina become damaged. They may leak fluid, bleed, or grow abnormally. These fragile new vessels can rupture easily, causing vitreous hemorrhage—where blood fills the vitreous cavity and blocks vision.
Patients often describe this experience as seeing dark clouds, cobwebs, or complete visual blackout in one eye. When bleeding does not clear on its own or when scar tissue forms and pulls on the retina (a condition called tractional retinal detachment), vitrectomy becomes necessary.
During surgery, the ophthalmologist removes the blood-filled vitreous gel and carefully eliminates scar tissue that may be tugging at the retina. Surgeons frequently apply laser treatment during the same procedure to seal abnormal vessels and prevent further bleeding.
Vitrectomy in diabetic patients is not merely about clearing vision—it’s about preventing permanent retinal damage. While surgery cannot cure diabetes, it can significantly preserve and sometimes restore functional vision.
Good blood sugar control after surgery is essential. Think of vitrectomy as repairing the damage, but daily diabetic management as preventing it from happening again.
Macular Hole and Macular Pucker
The macula is the central part of the retina responsible for sharp, detailed vision. When something goes wrong here, everyday tasks like reading, driving, or recognizing faces become challenging.
A macular hole develops when the vitreous pulls strongly on the macula, creating a small opening in the retinal tissue. Patients often notice blurred central vision or a dark spot in the middle of their sight. Straight lines may appear distorted.
In contrast, a macular pucker (also called an epiretinal membrane) occurs when a thin layer of scar tissue forms on the macula’s surface. This membrane contracts and wrinkles the retina, leading to wavy or distorted vision.
Vitrectomy is the primary treatment for both conditions. During the procedure, the surgeon removes the vitreous gel and carefully peels away the scar tissue or membrane using microscopic instruments. In cases of macular hole, a gas bubble is placed inside the eye to help the hole close properly.
Recovery requires patience. Some patients must maintain a face-down position for several days to allow the gas bubble to press gently against the macula, promoting healing. Vision improvement may take weeks or even months, but many patients experience significant functional gains.
These procedures highlight the precision of modern eye surgery—working on structures thinner than a sheet of paper, yet vital to clear vision.
Vitreous Hemorrhage
Vitreous hemorrhage refers to bleeding into the vitreous cavity. It can occur due to diabetes, retinal tears, trauma, or other vascular disorders. When blood fills the vitreous space, light cannot pass through clearly, leading to partial or complete vision loss.
In mild cases, the blood may gradually settle and be absorbed naturally. However, when bleeding is dense or persistent, waiting may not be an option. Prolonged hemorrhage can prevent the surgeon from examining and treating underlying retinal damage.
Vitrectomy removes the blood and restores optical clarity. More importantly, it allows the surgeon to identify and treat the source of bleeding—often with laser therapy. Early intervention reduces the risk of further complications, including retinal detachment.
Eye Trauma and Infections
Severe eye injuries can cause vitreous damage, bleeding, or foreign bodies inside the eye. Vitrectomy enables surgeons to remove debris, repair retinal tears, and restore internal eye structure.
In cases of endophthalmitis—a serious infection inside the eye—vitrectomy may be lifesaving for vision. Removing infected vitreous material helps reduce the bacterial load and allows antibiotics to work more effectively.
These emergency situations demonstrate how vitrectomy is not just elective surgery but sometimes a critical intervention.
Types of Vitrectomy Procedures
Pars Plana Vitrectomy
Pars plana vitrectomy (PPV) is the most common and widely performed type. The surgeon makes tiny incisions in the pars plana region of the eye—an area that allows safe access without damaging vital structures.
Through these micro-incisions, specialized instruments are inserted to cut and remove the vitreous gel. Modern PPV uses extremely small gauges (23, 25, or even 27-gauge systems), resulting in faster healing and minimal discomfort.
PPV is versatile and used for most retinal conditions, including detachment, macular disorders, and diabetic complications.
Anterior Vitrectomy
Anterior vitrectomy is performed when vitreous gel moves into the front portion of the eye, often during complicated cataract surgery or trauma. This procedure focuses on removing vitreous from the anterior chamber to prevent pressure issues and inflammation.
Although less extensive than pars plana vitrectomy, it remains a critical surgical skill.
Micro-Incision Vitrectomy Surgery (MIVS)
MIVS represents the evolution of vitreoretinal surgery. Using ultra-small instruments, surgeons can perform complex procedures with minimal tissue disruption.
Benefits include:
- Reduced surgical time
- Faster recovery
- Less postoperative discomfort
- Lower risk of complications
Modern vitrectomy has become significantly safer due to these technological advancements.
Pre-Operative Preparation
Medical Evaluation and Tests
Before surgery, patients undergo a thorough eye examination. This includes visual acuity testing, retinal imaging (such as OCT scans), and sometimes ultrasound if bleeding blocks visibility.
The medical team carefully reviews the patient’s medical history. Doctors ensure that conditions like high blood pressure or diabetes are under control before surgery. They may also require blood tests and clearance from the primary physician.
Preparation ensures safety and optimizes surgical outcomes.
Patient Instructions Before Surgery
Patients are typically advised to:
- Stop certain medications if instructed
- Avoid eating or drinking for several hours before surgery
- Arrange transportation home
- Discuss anesthesia options
Understanding the process reduces anxiety and improves cooperation during recovery.
Step-by-Step Vitrectomy Procedure
Anesthesia Administration
Vitrectomy is usually performed under local anesthesia with sedation. In complex cases, general anesthesia may be used.
Local anesthesia numbs the eye while the patient remains relaxed but awake. The goal is comfort without pain.
Removal of the Vitreous Gel
Using microscopic instruments, the surgeon removes the vitreous gel carefully. A vitrector—a tiny cutting device—breaks the gel into small fragments and suctions them out.
This step creates space and allows access to the retina.
Repairing Retinal Damage
The surgeon may perform laser therapy, peel membranes, or drain fluid depending on the condition. They customize each step according to the patient’s diagnosis.
Replacing the Vitreous
The vitreous cavity is filled with:
- Saline solution
- Gas bubble
- Silicone oil
Gas bubbles dissolve naturally over weeks. Silicone oil may require later removal.
The incisions are often self-sealing, requiring no stitches.
Recovery After Vitrectomy Surgery
Immediate Post-Operative Care
After surgery, the eye is covered with a protective shield. Mild discomfort, redness, and blurred vision are common initially.
Patients use prescribed eye drops to prevent infection and reduce inflammation.
Long-Term Healing Process
Vision improvement may take weeks or months. If the surgeon uses a gas bubble, patients must avoid air travel until it dissolves because altitude changes can dangerously increase eye pressure.
Follow-up appointments are essential to monitor healing.
Risks and Potential Complications
Like any surgery, vitrectomy carries risks.
Common Side Effects
- Temporary blurred vision
- Mild discomfort
- Increased eye pressure
- Cataract development over time
Rare but Serious Complications
- Retinal re-detachment
- Infection
- Severe bleeding
- Persistent vision loss
However, when performed by experienced retinal specialists, success rates are high.
Benefits and Success Rate of Vitrectomy
Vitrectomy has transformed retinal care. Success rates vary depending on the condition but often exceed 85–90% in many cases.
The primary benefits include:
- Restoration of visual clarity
- Prevention of blindness
- Relief from visual distortion
- Improved quality of life
Early intervention improves outcomes significantly.
Lifestyle Adjustments After Surgery
Positioning Requirements
Some patients must maintain specific head positions after surgery. This helps gas bubbles support retinal healing.
Travel and Activity Restrictions
Avoid:
- Air travel with gas bubble
- Heavy lifting
- Strenuous exercise
Gradual return to normal activities is encouraged under medical guidance.
Cost of Vitrectomy Surgery
Costs vary depending on:
- Geographic location
- Hospital facility
- Surgeon expertise
- Complexity of the condition
Insurance often covers medically necessary vitrectomy procedures.
When to Consult an Eye Specialist
Seek immediate medical care if you experience:
- Sudden flashes of light
- New floaters
- Vision loss
- Eye trauma
Early diagnosis prevents complications.
Conclusion
Vitrectomy operation is a highly advanced, vision-saving surgical procedure designed to treat complex retinal and vitreous disorders. From diabetic complications to retinal detachment, this microsurgical intervention restores clarity and protects long-term eye health. With modern techniques and experienced retinal specialists, outcomes continue to improve dramatically. Prompt consultation, proper preparation, and careful postoperative care remain essential for optimal recovery.
Author Details:
Dr. Sushruth Appajigowda holds a prominent position as a Cornea, Cataract, Glaucoma, and LASIK Surgeon in Bangalore. He serves as the chief Cataract and Refractive surgeon at Vijaya Nethralaya Eye Hospital, Nagarbhavi Bangalore. Renowned as one of the finest LASIK surgeons nationwide, he brings with him over 12+ years of experience across multiple LASIK platforms, including ZEISS, ALCON, SCHWIND, AMO, and Bausch and Lomb. Having successfully conducted over 5000 LASIK procedures, Dr. Sushruth holds the title of a Certified Refractive Surgeon and a Fellow of the All India Collegium Of Ophthalmology. Furthermore, he stands as a distinguished speaker at various National and International Forums, using his expertise to guide you in selecting the most suitable procedure based on your health requirements.

http://vijayanethralaya.com/link-in-bio/
FAQs
1. Is vitrectomy surgery painful?
The procedure is typically painless due to anesthesia. Mild discomfort may occur afterward but is manageable.
2. How long does vitrectomy surgery take?
Most procedures last between 1 to 2 hours, depending on complexity.
3. Will vision return to normal after vitrectomy?
Results vary based on the underlying condition, but many patients experience significant improvement.
4. How long does a gas bubble stay in the eye?
Gas bubbles usually dissolve within 2 to 8 weeks.
5. Can both eyes undergo vitrectomy at the same time?
Typically, surgeries are performed on one eye at a time for safety reasons.