Understanding Retinal Detachment
What Is Retinal Detachment?
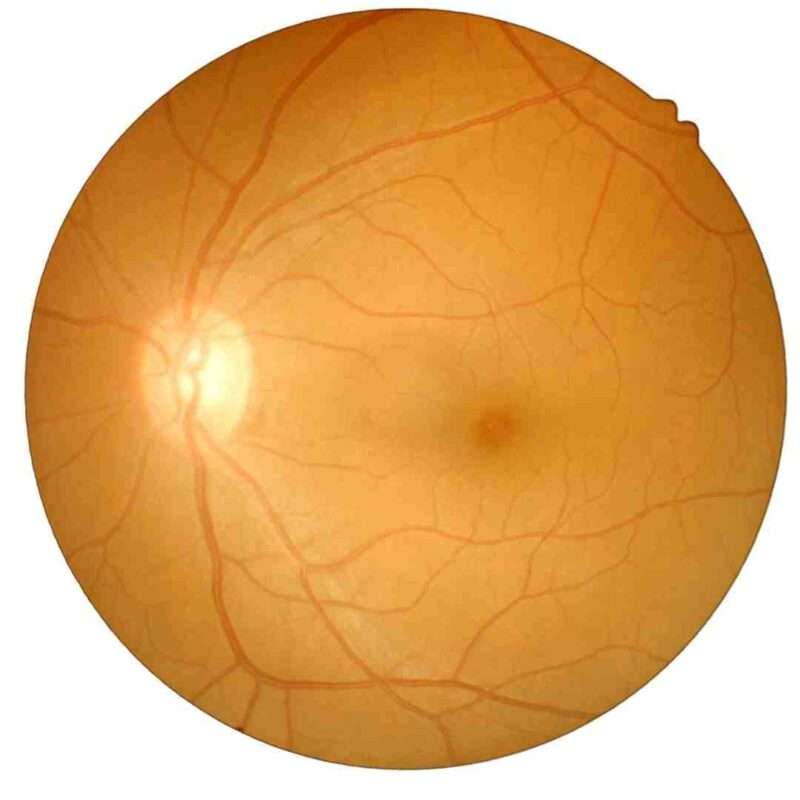
Retinal detachment is a serious eye condition that occurs when the retina, a thin layer of light-sensitive tissue at the back of the eye, becomes separated from its supporting layer. This separation prevents the retina from functioning properly, leading to blurry vision, flashes of light, or even sudden blindness if left untreated.
Unlike minor vision issues that develop gradually, retinal detachment is a medical emergency that requires immediate attention. Early diagnosis and treatment can make the difference between saving or losing one’s sight.
Anatomy of the Retina and Its Role in Vision
The retina acts like a camera film inside the eye. It captures light and converts it into electrical signals that the brain interprets as images. The macula, a central part of the retina, provides sharp vision needed for tasks like reading and driving.
When the retina detaches, its blood supply is cut off, and without prompt intervention, the cells can die, leading to permanent vision loss. This is why ophthalmologists emphasize the importance of recognizing early warning signs.
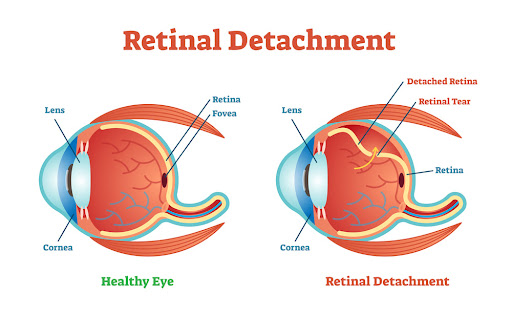
Types of Retinal Detachment
Rhegmatogenous Retinal Detachment
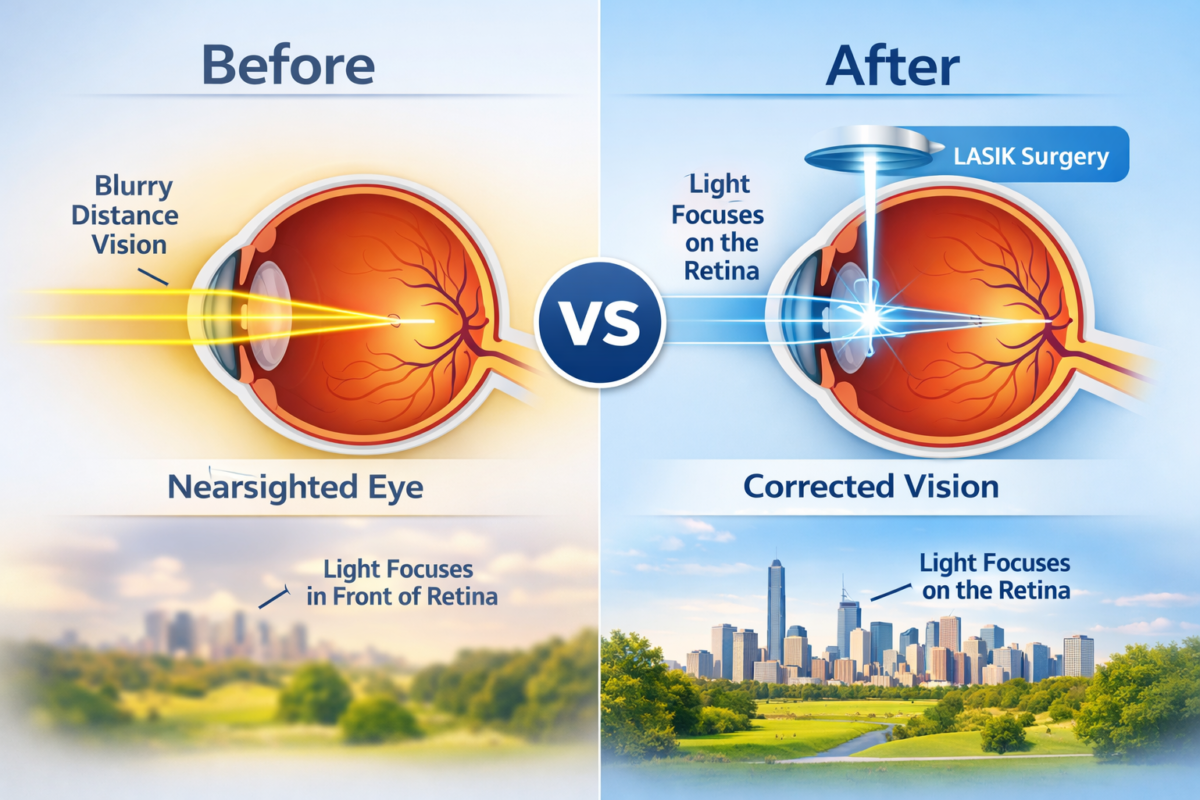
This is the most common type, caused by a tear or break in the retina. Fluid from the eye seeps through the tear, lifting the retina from the underlying tissue. It often occurs in people with severe myopia (nearsightedness) or after trauma.
Tractional Retinal Detachment
Seen more commonly in individuals with diabetic retinopathy, this type develops when scar tissue on the retina contracts, pulling it away from the back of the eye. It usually progresses more slowly than rhegmatogenous detachment.
Exudative (Serous) Retinal Detachment
Unlike the other two, this form occurs without a tear. Instead, fluid builds up beneath the retina due to inflammation, tumors, or vascular abnormalities. It’s less common but equally dangerous if untreated.
Causes and Risk Factors
Common Causes of Retinal Detachment
- Retinal tears from aging changes in the vitreous gel.
- Eye injuries leading to trauma.
- Previous eye surgeries such as cataract removal.
- Chronic diseases like diabetes.
Risk Factors: Who Is Most at Risk?
Age and Eye Health
Retinal detachment is more common in individuals over 50 years old due to natural eye changes.
Family History and Genetics
A family history of retinal detachment increases one’s risk significantly.
Trauma and Eye Injuries
Sports injuries, accidents, or physical trauma can trigger detachment.
Other Eye Conditions
- Severe myopia (nearsightedness)
- Complications after cataract surgery
- Conditions like diabetic retinopathy or uveitis
Warning Signs and Symptoms
Early Symptoms of Retinal Detachment
- Sudden appearance of floaters (black spots or cobweb-like shadows).
- Flashes of light, especially at night.
- Blurred or distorted vision.
- A shadow or curtain effect across part of the visual field.
When to Seek Emergency Medical Help
If you notice sudden floaters, light flashes, or loss of peripheral vision, seek urgent ophthalmic care. Delay in treatment can result in irreversible blindness.
Diagnosis of Retinal Detachment
Ophthalmic Examination
The first step in diagnosing retinal detachment is a comprehensive eye exam conducted by an ophthalmologist. Using specialized equipment such as an ophthalmoscope, the doctor examines the retina for tears, holes, or areas of detachment. A dilated eye exam allows for a clearer view of the back of the eye, making it easier to spot abnormalities.
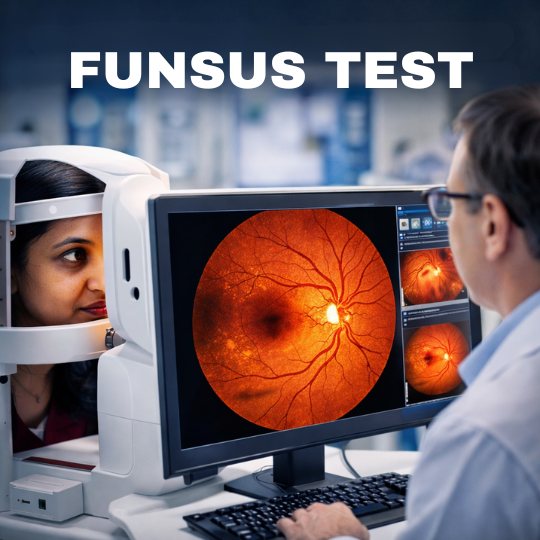
Imaging Tests: OCT, Ultrasound, and Fundus Photography
- Optical Coherence Tomography (OCT): Provides high-resolution cross-sectional images of the retina, useful for detecting subtle detachments.
- Ocular Ultrasound: Helps confirm detachment when the retina is obscured by bleeding inside the eye (vitreous hemorrhage).
- Fundus Photography: Captures detailed images of the retina for documentation and monitoring.
A timely diagnosis is crucial, as early intervention dramatically increases the chances of saving vision.
Treatment Options for Retinal Detachment
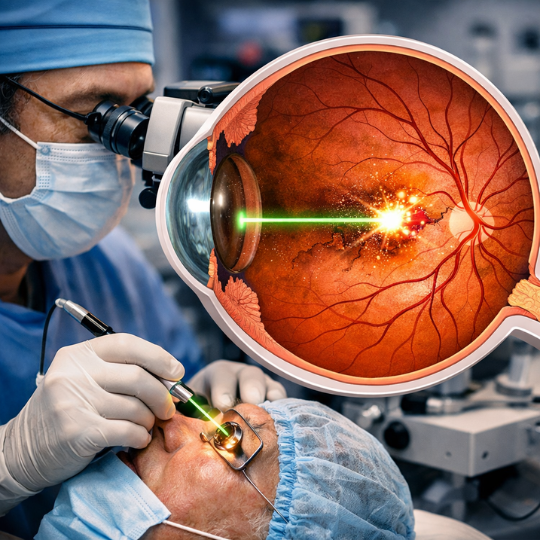
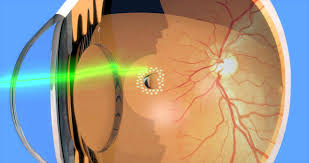
Laser Therapy (Photocoagulation)
Laser therapy seals retinal tears before detachment spreads. This outpatient procedure uses a laser beam to create scar tissue, securing the retina to its underlying layer.
Cryopexy (Freezing Therapy)
In cryopexy, a freezing probe is applied to the outer eye surface, freezing the area around the retinal tear. Like laser therapy, it helps form scar tissue that “glues” the retina in place.
Pneumatic Retinopexy
In this minimally invasive technique, a gas bubble is injected into the eye to push the retina back against the wall. Patients are usually required to maintain a specific head position for several days to keep the bubble in place.
Scleral Buckling Surgery
A silicone band is placed around the eye’s outer surface to relieve pressure and push the eye wall against the retina. This method has been used for decades and remains highly effective.
Vitrectomy
A more advanced surgical option, vitrectomy involves removing the vitreous gel from the eye and replacing it with gas or silicone oil. This approach is often used for complex or severe detachments.
Recovery and Post-Surgery Care
Short-Term Recovery Process
- Vision may be blurry for several weeks.
- Patients are often advised to avoid strenuous activity.
- Eye drops are prescribed to prevent infection and reduce inflammation.
- If a gas bubble was used, patients must avoid air travel until the bubble dissolves.
Long-Term Outlook for Patients
Most patients regain some or all of their vision if treated early. However, vision may not return to normal if the macula (central retina) was affected. Regular follow-up visits ensure proper healing and monitor for recurrence.
Complications if Left Untreated
Vision Loss and Blindness
Untreated retinal detachment almost always leads to permanent vision loss. The retina’s cells cannot survive long without their blood supply.
Secondary Eye Conditions
- Glaucoma due to increased eye pressure.
- Cataracts developing as a result of surgery or trauma.
- Recurrent detachments, which may require multiple surgeries.
Prevention and Lifestyle Tips
Regular Eye Exams
Routine eye check-ups, especially for those at high risk, can catch early signs of retinal tears before detachment occurs.
Managing Chronic Conditions
Keeping conditions like diabetes and hypertension under control lowers the risk of retinal damage.
Eye Safety and Protective Measures
- Wearing protective eyewear during sports or hazardous activities.
- Avoiding direct trauma to the eye whenever possible.
Living with Retinal Detachment
Coping Mechanisms for Vision Impairment
- Using magnifying devices or digital aids to improve reading ability.
- Rearranging home lighting to minimize glare.
- Learning orientation and mobility skills if vision loss is severe.
Support Groups and Resources
Connecting with others through support groups or counseling helps patients adapt emotionally. Resources from organizations such as the American Academy of Ophthalmology (AAO) provide guidance and education.
Retinal Detachment in Children vs. Adults
Pediatric Retinal Detachment
Rare but serious, pediatric detachment is often linked to trauma, congenital eye conditions, or retinopathy of prematurity. Treatment is similar but can be more challenging due to the delicate nature of developing eyes.
Age-Related Retinal Detachment
In adults, especially over 50, age-related changes in the vitreous gel increase the risk of retinal tears. Regular monitoring is essential for this group.
Conclusion
Retinal detachment is a sight-threatening condition that demands urgent medical attention. With timely diagnosis and modern treatments such as laser therapy, scleral buckling, and vitrectomy, most patients can preserve their vision.
The best defense lies in awareness and prevention. Knowing the warning signs—flashes of light, floaters, and sudden vision changes—can help you act before irreversible damage occurs.
FAQs About Retinal Detachment
1. Can retinal detachment heal on its own?
No. Retinal detachment does not heal without medical treatment and requires surgical or laser intervention.
2. How fast does retinal detachment progress?
It can progress rapidly within hours or days, making early diagnosis and treatment critical.
3. Is retinal detachment painful?
No, it’s usually painless. However, the vision symptoms are sudden and alarming.
4. Can both eyes be affected?
Yes, people who experience detachment in one eye are at higher risk of developing it in the other.
5. How successful are surgeries for retinal detachment?
Success rates are high, with 80–90% of patients achieving reattachment after a single surgery.
6. Can lifestyle changes prevent retinal detachment?
While not all cases are preventable, regular eye exams, protective eyewear, and managing health conditions can reduce risk.