Introduction:
Living with diabetes is like juggling plates—you’re constantly balancing blood sugar, diet, medications, and long-term health. Now add vision problems to the mix, and things can feel overwhelming fast. Cataracts are one of the most common eye conditions affecting diabetic patients, and the idea of surgery can spark fear, confusion, and a hundred unanswered questions. The good news? Cataract surgery is not only possible for diabetic patients—it’s often life-changing when done at the right time and with proper care.
This guide breaks everything down in plain English. No medical jargon overload. No sugarcoating. Just clear, practical information to help you understand cataract surgery for diabetic patients from start to finish—what’s different, what to expect, and how to protect your vision long-term.
Understanding Cataracts and Diabetes:
Cataracts and diabetes often walk hand in hand. If you’ve been managing diabetes for years, your eyes have likely felt the impact—even if you didn’t notice it at first.
What Is a Cataract?
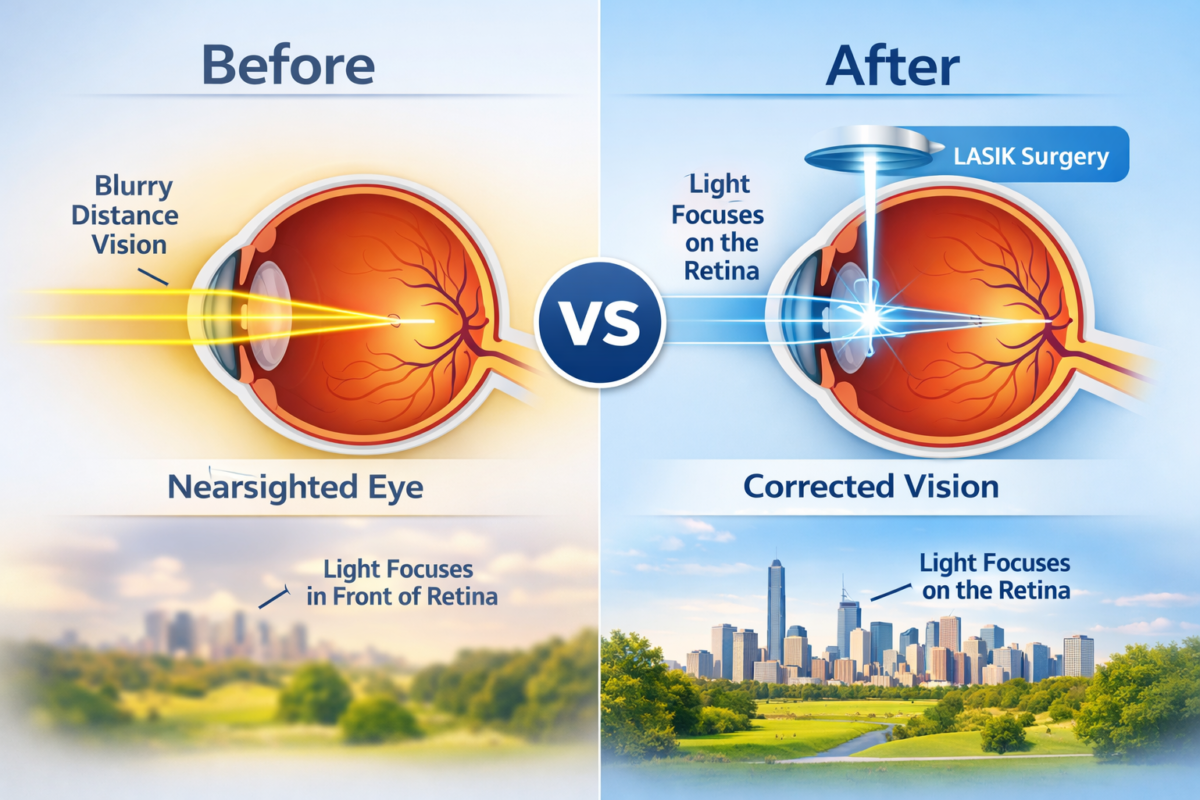
A cataract forms when the natural lens of your eye becomes cloudy. Think of your eye’s lens like a camera lens. When it’s clear, light passes through easily, producing sharp images. When it clouds up, everything looks foggy, dull, or blurred—like trying to see through a dirty windshield.
Cataracts usually develop slowly. One day you’re squinting at street signs, and before you know it, reading or driving at night feels impossible. While cataracts are common with aging, diabetes speeds up this process significantly.
How Diabetes Affects Eye Health
Diabetes affects blood vessels throughout the body, and the eyes are no exception. High blood sugar damages tiny blood vessels in the retina, disrupts fluid balance in the lens, and increases oxidative stress—all of which contribute to cataract formation.
When glucose levels remain high, excess sugar enters the lens and turns into sorbitol. This substance draws in water, causing the lens to swell and become cloudy. Over time, repeated swelling and shrinking permanently damages lens clarity.
Why Cataracts Develop Faster in Diabetic Patients
Here’s the blunt truth: diabetics develop cataracts earlier and more aggressively than non-diabetics. A person without diabetes might develop cataracts in their 60s or 70s. Diabetic patients often notice symptoms in their 40s or 50s—or even earlier.
Poor blood sugar control accelerates lens aging, making cataracts denser and more visually disruptive. That’s why regular eye exams aren’t optional for diabetics—they’re essential.
The Link Between Blood Sugar Levels and Lens Damage
Stable blood sugar acts like a protective shield for your eyes. Fluctuating glucose levels cause constant stress on the lens, leading to faster clouding. Even short-term spikes can temporarily blur vision, which many diabetics mistake for “just a bad day.”
Over time, these fluctuations leave permanent damage. That’s why ophthalmologists often emphasize blood sugar control as part of cataract treatment—not just before surgery, but for life.
Types of Cataracts Common in Diabetic Patients:
Not all cataracts are created equal. Diabetic patients tend to develop certain types more frequently, and understanding them helps explain why vision can deteriorate so quickly.
Nuclear Cataracts
Nuclear cataracts form in the center of the lens and gradually turn it yellow or brown. While common in aging, diabetes accelerates their progression. Colors may appear faded, and reading becomes increasingly difficult.
Cortical Cataracts
Cortical cataracts start at the edges of the lens and move inward. They create glare, halos, and contrast issues—especially at night. Diabetics often experience these symptoms earlier due to metabolic changes in the lens.
Posterior Subcapsular Cataracts
This is where diabetes really shows its hand. Posterior subcapsular cataracts develop at the back of the lens and progress rapidly. Even a small cataract here can cause major vision problems.
Why Posterior Subcapsular Cataracts Are More Aggressive in Diabetes
These cataracts interfere directly with light entering the eye, making reading, bright light, and night driving extremely difficult. Diabetic patients are particularly prone to this type because high glucose levels disrupt lens cell metabolism near the posterior capsule.
The result? Faster vision loss and earlier need for surgery.
Symptoms of Cataracts in Diabetic Patients:
Cataract symptoms can sneak up quietly or hit hard and fast—especially for diabetics.
Early Warning Signs
- Blurry or cloudy vision
- Increased glare from lights
- Difficulty reading small print
- Colors appearing dull or yellow
- Frequent changes in eyeglass prescription
Vision Changes Unique to Diabetics
Diabetic patients often notice fluctuating vision—clear one day, blurry the next. This can make cataracts harder to detect early, as symptoms overlap with blood sugar fluctuations.
When Symptoms Should Never Be Ignored:
If vision loss interferes with daily life, driving, work, or safety, it’s time to act. Sudden vision changes, severe glare, or rapid decline should trigger an immediate eye exam.
Ignoring symptoms doesn’t just delay surgery—it increases the risk of complications later.
Importance of Early Diagnosis
Early diagnosis is like catching a small fire before it burns the house down.
Routine Eye Exams for Diabetics:
Diabetics should have a comprehensive dilated eye exam at least once a year—more often if recommended. These exams detect cataracts, diabetic retinopathy, and macular edema early.
Diagnostic Tests Used Before Cataract Surgery
- Visual acuity tests
- Slit-lamp examination
- Retinal imaging (OCT)
- Intraocular pressure measurement
Role of Retinal Evaluation Before Surgery
Before cataract surgery, the retina must be evaluated carefully. Conditions like diabetic retinopathy can affect surgical outcomes, so managing retinal issues first is crucial.
Is Cataract Surgery Safe for Diabetic Patients?
This is the million-dollar question—and the answer is reassuring.
General Safety Overview
Yes, cataract surgery is generally safe for diabetic patients. It’s one of the most commonly performed surgeries worldwide, with high success rates when proper precautions are taken.
How Modern Surgical Techniques Reduce Risk
Advances like small-incision surgery, improved intraocular lenses, and better medications have dramatically reduced complications. Surgeons now tailor procedures specifically for diabetic eyes.
Success Rates Compared to Non-Diabetic Patients
When diabetes is well-controlled and retinal health is managed, visual outcomes can be nearly as good as those in non-diabetic patients. The key lies in preparation and follow-up.
Pre-Surgery Evaluation and Preparation:
Preparation isn’t just paperwork—it’s protection for your vision.
Blood Sugar Control Before Surgery
Good glucose control reduces inflammation, speeds healing, and lowers infection risk. Surgeons often coordinate with primary care doctors or endocrinologists to ensure stable levels before surgery.
Managing Diabetic Retinopathy
If retinopathy is present, it may need treatment—such as laser therapy or injections—before cataract surgery. Addressing this first improves outcomes and prevents worsening after surgery.
Preoperative Tests and Imaging
Advanced imaging helps surgeons plan lens selection, incision placement, and surgical technique tailored to diabetic eyes.
Medications to Adjust Before Surgery
Some medications may need adjustment before surgery. Always follow your doctor’s instructions—guessing here can lead to complications.
Choosing the Right Time for Cataract Surgery:
Timing isn’t about waiting for blindness—it’s about quality of life.
When Surgery Becomes Necessary
If cataracts interfere with daily activities, work, or safety, surgery is usually recommended. Waiting too long can make surgery more difficult.
Risks of Delaying Cataract Surgery
Advanced cataracts are harder to remove and increase the risk of inflammation, pressure spikes, and retinal complications—especially in diabetics.
Coordinating with Diabetes Management
Surgery should be scheduled when blood sugar is stable and other diabetic complications are under control.
Types of Cataract Surgery for Diabetic Patients:
Surgical technique matters more for diabetic eyes.
Phacoemulsification
This is the most common method. Ultrasound breaks the cataract into tiny pieces, which are removed through a small incision. It offers faster healing and less inflammation.
Extracapsular Cataract Extraction
Used for very dense cataracts, this method involves a larger incision. It’s less common today but still effective in certain cases.
Laser-Assisted Cataract Surgery
Lasers improve precision and reduce trauma, which can benefit diabetic patients with sensitive eyes.
Which Method Is Best for Diabetics?
Most diabetics do well with phacoemulsification or laser-assisted surgery. The choice depends on cataract severity and overall eye health.
Intraocular Lens (IOL) Options for Diabetic Patients:
Choosing the right lens is like choosing the right tires for a car—it affects performance long after surgery.
Monofocal Lenses
These provide clear vision at one distance and are often recommended for diabetics due to reliability and fewer visual side effects.
Multifocal Lenses
While appealing, these lenses may not be ideal for diabetics with retinal issues, as they can reduce contrast sensitivity.
Toric Lenses
Perfect for correcting astigmatism, toric lenses can improve overall visual quality.
Special Considerations for Diabetics
Retinal health plays a major role in lens selection. Surgeons often prioritize clarity and contrast over convenience.
Cataract Surgery and Diabetic Retinopathy:
This relationship requires careful handling.
How Surgery Affects Retinopathy
Cataract surgery can temporarily worsen diabetic retinopathy due to inflammation. However, with proper management, this risk is minimized.
Managing Retinal Swelling (Macular Edema)
Anti-inflammatory eye drops or injections may be used before and after surgery to prevent swelling.
Combined Treatments with Retina Specialists
Many patients benefit from a team approach involving both cataract and retina specialists.
Risks and Complications in Diabetic Patients:
Every surgery has risks—but knowledge reduces fear.
Increased Risk of Infection
Diabetes slightly increases infection risk, but strict sterile techniques and medications keep this rare.
Inflammation and Slow Healing
Healing may take longer, but proper medication and follow-up help manage this effectively.
Postoperative Macular Edema
This is one of the most common concerns and is closely monitored after surgery.
How These Risks Are Managed
Modern medications, imaging, and close monitoring dramatically reduce complication rates.
The Cataract Surgery Procedure: Step by Step:
Knowing what happens reduces anxiety.
What Happens on Surgery Day
The procedure is outpatient, meaning you go home the same day.
Anesthesia and Comfort
Local anesthesia ensures you’re comfortable and pain-free.
Duration and What the Patient Experiences
Surgery typically takes 15–30 minutes, with minimal discomfort.
Postoperative Care and Recovery:
Recovery is where discipline pays off.
Immediate Aftercare
Vision improves quickly, but protection and rest are essential.
Eye Drops and Medications
Anti-inflammatory and antibiotic drops prevent infection and swelling.
Blood Sugar Management After Surgery
Stable glucose levels speed healing and protect vision.
Expected Recovery Timeline
Most patients resume normal activities within days, with full recovery over weeks.
Long-Term Vision Outcomes for Diabetic Patients
The payoff is worth it.
Vision Improvement Expectations
Clearer, brighter vision is common—often better than patients expect.
Factors That Influence Final Results
Retinal health, blood sugar control, and follow-up care all matter.
Maintaining Eye Health After Surgery
Regular exams remain essential even after successful surgery.
Lifestyle Tips to Protect Vision After Cataract Surgery:
Think of surgery as a reset—not a cure.
Diet and Blood Sugar Control
Healthy eating protects both eyes and overall health.
Eye Protection and Hygiene
Sunglasses, cleanliness, and avoiding eye strain help preserve results.
Importance of Regular Follow-Ups
Consistency prevents future problems.
Cost and Insurance Coverage
Understanding costs avoids surprises.
Average Cost of Cataract Surgery
Costs vary by location and lens choice.
Insurance and Medicare Considerations
Most plans cover standard surgery and monofocal lenses.
Additional Costs for Advanced Lenses
Premium lenses often involve out-of-pocket expenses.
Author Details:
Dr. Sushruth Appajigowda holds a prominent position as a Cornea, Cataract, Glaucoma, and LASIK Surgeon in Bangalore. He serves as the chief Cataract and Refractive surgeon at Vijaya Nethralaya Eye Hospital, Nagarbhavi Bangalore. Renowned as one of the finest LASIK surgeons nationwide, he brings with him over 12+ years of experience across multiple LASIK platforms, including ZEISS, ALCON, SCHWIND, AMO, and Bausch and Lomb. Having successfully conducted over 5000 LASIK procedures, Dr. Sushruth holds the title of a Certified Refractive Surgeon and a Fellow of the All India Collegium Of Ophthalmology. Furthermore, he stands as a distinguished speaker at various National and International Forums, using his expertise to guide you in selecting the most suitable procedure based on your health requirements.

http://vijayanethralaya.com/link-in-bio/
Conclusion:
Cataract surgery for diabetic patients isn’t something to fear—it’s something to prepare for wisely. With proper blood sugar control, careful surgical planning, and committed follow-up care, diabetic patients can achieve excellent visual outcomes. Clear vision isn’t just about seeing better—it’s about living better, safer, and more confidently. When managed correctly, cataract surgery becomes not just a medical procedure, but a turning point toward a brighter, clearer future.
FAQs:
1. Can diabetics undergo cataract surgery safely?
Yes, with proper preparation and blood sugar control, cataract surgery is safe and effective.
2. Does cataract surgery worsen diabetic retinopathy?
It can temporarily affect it, but proper management minimizes risks.
3. How long does recovery take for diabetic patients?
Most recover within weeks, though healing may be slightly slower.
4. Is laser cataract surgery better for diabetics?
It can offer benefits, but suitability depends on individual eye health.
5. How can diabetics protect their vision after surgery?
By controlling blood sugar, attending follow-ups, and maintaining a healthy lifestyle.