Is Cataract Surgery Safe for Diabetics? Everything You Need to Know in 2025
Cataract surgery is one of the most common and successful eye procedures performed worldwide. However, when it comes to patients with diabetes, many people often wonder, is cataract surgery safe for diabetics?
The short answer is yes, cataract surgery is generally safe for diabetics when managed carefully under the supervision of an experienced ophthalmologist. Yet, diabetic patients need special preoperative and postoperative care to ensure optimal results.
In this detailed guide, we’ll explore everything diabetics should know before undergoing cataract surgery—including risks, preparation, recovery, and how to protect long-term vision health.

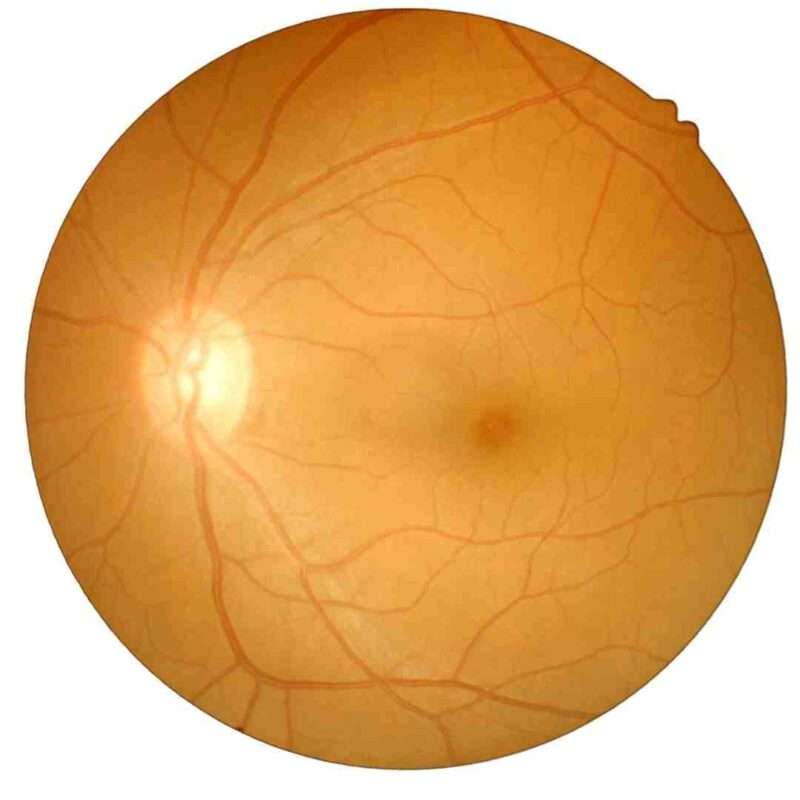
Understanding Cataracts and Diabetes
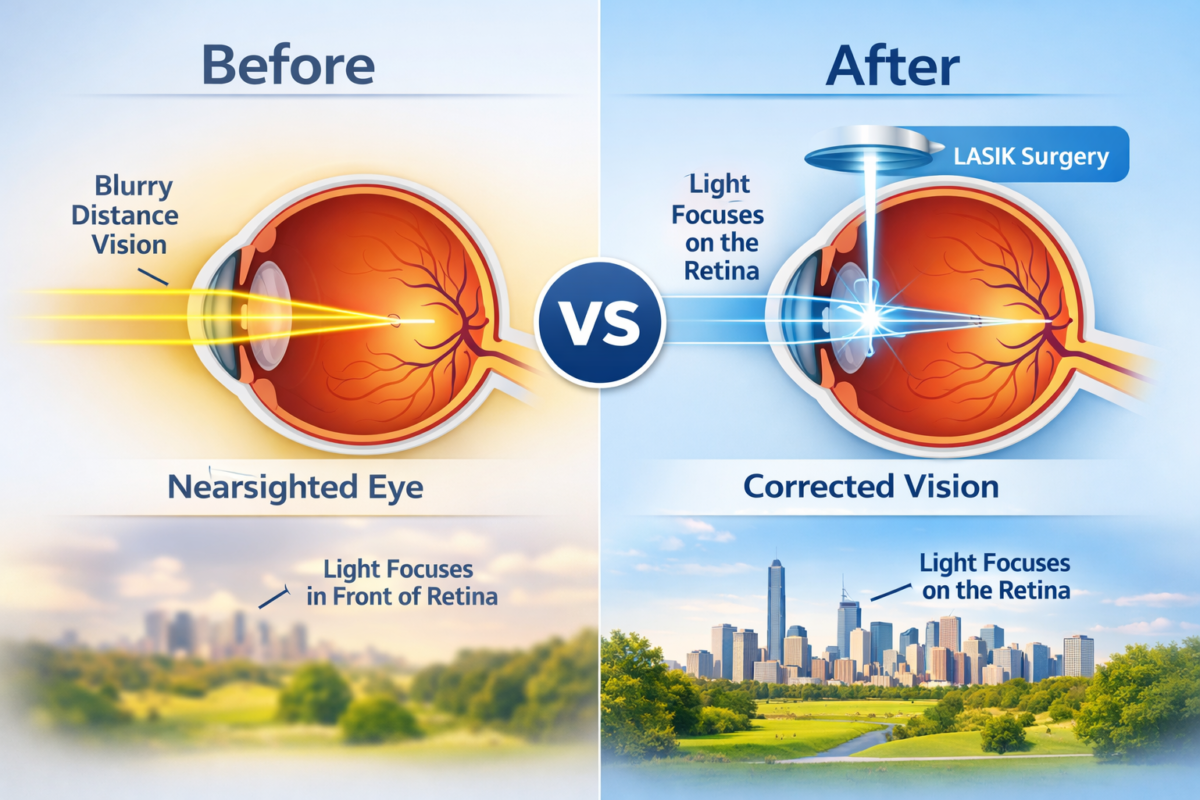
A cataract occurs when the natural lens of your eye becomes cloudy, leading to blurred vision, glare, and difficulty seeing at night. People with diabetes tend to develop cataracts earlier, and they progress faster than in non-diabetics.
How Diabetes Causes Cataracts
High blood sugar levels can cause chemical changes in the eye lens, leading to:
- Lens swelling due to sugar absorption
- Protein clumping, which clouds the lens
- Oxidative stress, damaging lens fibers
This makes diabetics two to five times more likely to develop cataracts than non-diabetics—and often at a younger age.
Is Cataract Surgery Safe for Diabetic Patients?
Yes, cataract surgery is safe for diabetics when performed with proper planning, modern technology, and postoperative care.
However, diabetes can complicate both the surgery and healing process if blood sugar levels are poorly controlled. That’s why choosing the right eye surgeon and hospital plays a crucial role in achieving excellent outcomes.
Surgeons at Vijaya Nethralaya Super Speciality Eye Hospital in Bangalore use advanced phacoemulsification and femtosecond laser-assisted techniques to perform cataract surgeries for diabetic patients, ensuring minimal trauma, faster recovery, and greater precision.

Risks of Cataract Surgery in Diabetic Patients
While the surgery itself is safe, diabetics face a slightly higher risk of certain postoperative complications. Understanding these risks can help manage expectations and outcomes effectively.
Macular Edema (Swelling in the Retina)
After surgery, fluid accumulation can cause diabetic macular edema (DME), leading to blurred central vision. Presurgical retinal assessment helps prevent this.
Slower Healing
High blood sugar can delay wound healing, making recovery slower than in non-diabetic patients.
Infection (Endophthalmitis)
Although rare, uncontrolled diabetes increases infection risks. Strict hygiene and antibiotics reduce this possibility.
Diabetic Retinopathy Progression
Existing diabetic retinopathy can worsen after surgery due to inflammation. This is why a comprehensive retina check before surgery is essential.
Fluctuating Vision Post-Surgery
Temporary changes in blood sugar can cause blurred vision for a few days post-surgery until levels stabilize.
How Diabetics Can Prepare for Cataract Surgery
Proper preoperative preparation is the key to success for diabetic cataract patients.
1. Control Blood Sugar Levels
Ensure HbA1c (3-month average sugar) is below 7% before surgery. Stable glucose reduces complications.
2. Comprehensive Eye Check-Up
Your ophthalmologist will perform:
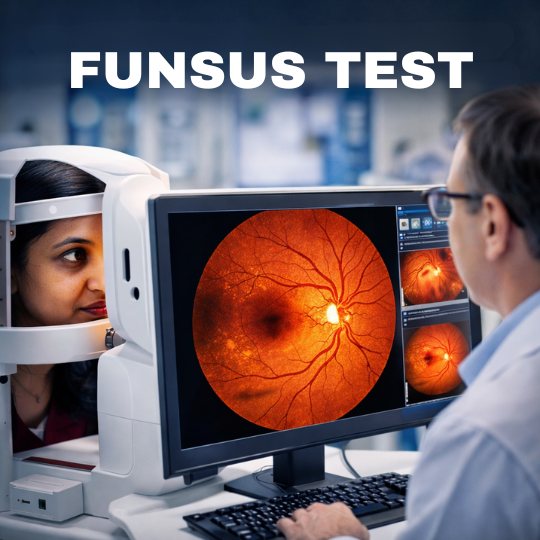
- Retinal examination (OCT or fundus check)
- Corneal and lens measurement
- Intraocular pressure assessment
If diabetic retinopathy or macular edema is detected, it must be treated before surgery.
3. Discuss Medications
Inform your doctor about all medications—especially insulin or oral hypoglycemics—so doses can be adjusted on the day of surgery.
4. Preoperative Retina Treatment
If diabetic retinopathy is active, laser therapy or anti-VEGF injections may be done before cataract removal.
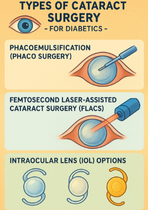
Types of Cataract Surgery for Diabetics
Modern cataract surgery has evolved to become minimally invasive, painless, and highly precise. Here are the most common options:
1. Phacoemulsification (Phaco Surgery)
The most widely performed technique uses ultrasound energy to break and remove the cataract.
Benefits:
- Small incision (2–3 mm)
- Quick healing
- No stitches required
- Excellent visual outcome
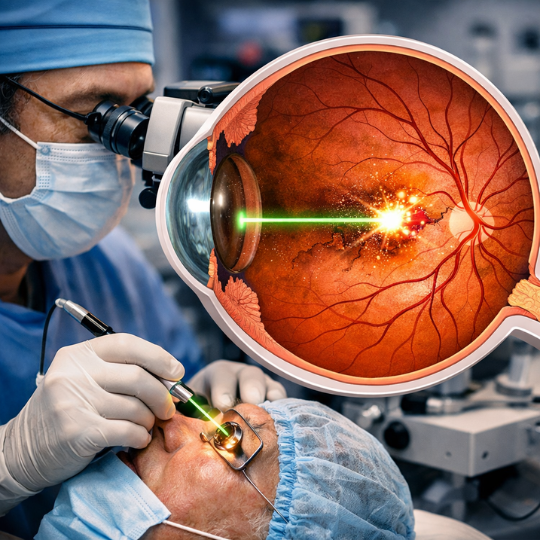
2. Femtosecond Laser-Assisted Cataract Surgery (FLACS)
A bladeless laser surgery that offers superior precision and minimal eye stress.
Benefits:
- Ideal for diabetics with sensitive eyes
- Accurate incision and lens placement
- Reduced inflammation
3. Intraocular Lens (IOL) Options
After cataract removal, an artificial lens (IOL) is implanted.
For diabetics, monofocal lenses are preferred, as they provide clear distance vision and better retinal visualization if further diabetic eye treatment is needed.
During the Surgery: What Happens
Cataract surgery is a day care procedure—meaning you can go home the same day.
- The eye is numbed using drops or local anesthesia.
- The cloudy lens is removed using phacoemulsification or laser technology.
- A new IOL is implanted.
- No stitches are required, and the entire process takes 10–15 minutes.
At Vijaya Nethralaya Super Speciality Eye Hospital, all diabetic cataract procedures are guided by microscopic precision, advanced imaging, and sterile protocols, ensuring patient safety at every step.
Post-Surgery Care for Diabetic Patients
Postoperative care is critical to ensure smooth healing and maintain healthy vision.
1. Monitor Blood Sugar Levels
Keep your sugar levels stable—high glucose delays healing and increases infection risk.
2. Use Prescribed Eye Drops
Antibiotic and anti-inflammatory drops should be used as directed to prevent inflammation.
3. Avoid Rubbing the Eye
Even minor pressure can disrupt the incision site or displace the new lens.
4. Protect Your Eyes
Use protective glasses outdoors to prevent dust and UV damage.
5. Eat a Balanced Diet
Include antioxidants (vitamin C, E, lutein, and zinc) to promote lens and retinal health.
6. Follow Up Regularly
Attend all scheduled checkups. Your doctor will monitor for signs of:
- Macular edema
- Infection
- Retinopathy progression
Recovery Timeline After Cataract Surgery
Most diabetics experience improved vision within a few days. However, recovery may take slightly longer depending on overall health and sugar control.
| Timeline | What to Expect |
|---|---|
| Day 1–3 | Mild irritation or tearing, vision slightly blurred |
| 1 Week | Vision begins to clear up |
| 2–4 Weeks | Most activities can be resumed |
| 6 Weeks | Final vision stabilizes |
Your ophthalmologist will guide you when it’s safe to drive, work, or resume heavy activities.
Tips to Protect Vision Long-Term
Even after successful cataract surgery, diabetics must stay vigilant to protect their eyes from future complications.
Maintain Blood Sugar & Blood Pressure
Keep both under control to prevent retinopathy or macular edema.
Eat Eye-Healthy Foods
Include leafy greens, citrus fruits, omega-3s, and nuts in your diet.
Stay Active
Exercise improves blood circulation and helps control diabetes.
Regular Eye Checkups
Visit your ophthalmologist every 6–12 months to monitor retinal health.
Take Medications on Time
Never skip your diabetes medications or insulin—stability is key.
Why Choose Vijaya Nethralaya Super Speciality Eye Hospital for Diabetic Cataract Surgery
At Vijaya Nethralaya Super Speciality Eye Hospital, Bangalore, diabetic cataract patients receive personalized, evidence-based care from experienced cataract and retina specialists.
Our Expertise Includes:
- Advanced phaco and laser cataract systems
- Comprehensive diabetic eye evaluations (OCT, fundus imaging)
- Integrated retina and cataract management
- Tailored pre- and postoperative monitoring
- Patient education for long-term diabetic eye care
Our mission is not just to restore your vision but also to protect it for life.
When to Visit an Eye Doctor
If you are diabetic and experience any of the following, schedule an eye check immediately:
- Blurred or cloudy vision
- Sensitivity to light
- Difficulty reading or night driving
- Seeing halos or glare around lights
Early diagnosis and timely surgery prevent permanent vision loss.

Conclusion: Cataract Surgery Can Be Safe and Successful for Diabetics
To sum it up—cataract surgery is safe for diabetics when blood sugar is well controlled, and the surgery is performed by experienced ophthalmologists using modern technology.
With the right hospital, like Vijaya Nethralaya Super Speciality Eye Hospital in Bangalore, diabetic patients can expect:
- Sharp, clear vision
- Minimal risk of complications
- Faster recovery
- Long-lasting eye health
Don’t delay your eye check-up. Early evaluation ensures timely treatment and better vision outcomes.
FAQs
1. Can diabetics have cataract surgery safely?
Yes, with controlled blood sugar and professional care, diabetics can undergo cataract surgery safely.
2. How long does it take for a diabetic to recover after cataract surgery?
Most patients recover within 4–6 weeks, though healing may take slightly longer if sugar levels fluctuate.
3. Will cataract surgery cure diabetic retinopathy?
No. Cataract surgery improves lens clarity but doesn’t treat diabetic retinopathy — that needs separate management.
4. Can both eyes be operated on the same day?
Usually, doctors recommend doing one eye at a time to ensure proper healing and minimize infection risk.
5. How can I prevent cataracts from developing faster if I’m diabetic?
Maintain healthy blood sugar, eat antioxidant-rich foods, wear UV-protected glasses, and get regular eye checkups.